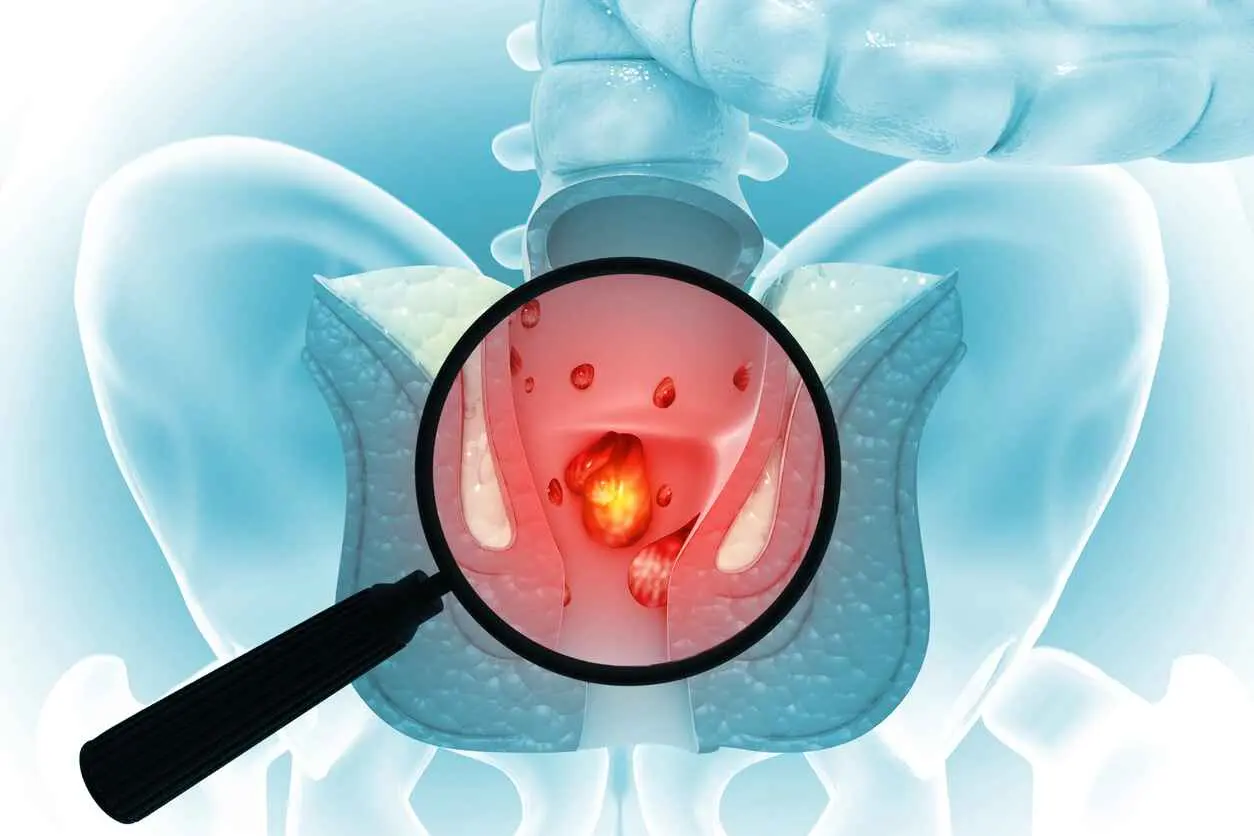
Causes Of Hemorrhoids And Tips For Prevention
Hemorrhoids occur when veins near the anus swell, typically as a result of straining during bowel movements or due to constipation. Some forms of haemorrhoids can lead to intense pain.
What Are Haemorrhoids?
Hemorrhoids, also known as piles, are swollen veins that can form around the anus or in the lower rectum. By the age of 50, about half of adults will have experienced symptoms of haemorrhoids.
They come in two types: internal, which forms inside the rectum, and external, which develops outside the anus. External haemorrhoids are more common and can cause significant discomfort, including pain, intense itching, and trouble sitting. However, they are treatable conditions.
What Are The Symptoms Of Haemorrhoids?
The symptoms of haemorrhoids vary depending on the type:
Internal haemorrhoids may lead to:
- Blood on toilet paper after a bowel movement.
- Skin protruding from the anus during bowel movements.
Symptoms of external haemorrhoids include:
- Severe itching around the anus.
- Uncomfortable lumps or swelling near the anus.
- Pain or aches around the anus, particularly when sitting.
Often, haemorrhoids do not cause pain. However, external haemorrhoids can sometimes develop a blood clot, resulting in a thrombosed haemorrhoid, which can be painful. Internal haemorrhoids might prolapse, meaning they don't retract back inside the anus, and this can also cause significant discomfort.
While haemorrhoids can be uncomfortable, they are not life-threatening and frequently resolve on their own without treatment. However, if you notice bleeding or black bowel movements, it's essential to consult a doctor, as these symptoms can be indicative of conditions other than haemorrhoids. Also, if haemorrhoids persist for more than a week despite home treatment, medical advice should be sought.
What Are The Causes And Risk Factors For Haemorrhoids?
Haemorrhoids develop due to excessive pressure on the veins near the anus. Factors that can contribute to this condition include:
- Straining while passing stools.
- Sitting for extended periods, particularly on the toilet.
- Experiencing ongoing constipation or diarrhoea.
- A family history of haemorrhoids.
- Regularly engaging in heavy lifting or activities that strain the body.
- Being overweight.
- Anal intercourse, which can aggravate hemorrhoids.
- Pregnancy, as an enlarged uterus, can press on the vein in the colon.
- Being over 50 years of age.
How Are Haemorrhoids Diagnosed?
Diagnosing haemorrhoids often begins with a visual examination of the anus. A digital rectal exam may be performed to confirm the diagnosis, where a healthcare professional inserts a gloved, lubricated finger into the rectum.
Additional tests like anoscopy, sigmoidoscopy, or colonoscopy might be recommended depending on individual risk factors for gastrointestinal diseases. These procedures involve using a small camera to detect any abnormalities in the anus, rectum, or colon. An anoscopy focuses on the inside of the anus, a sigmoidoscopy examines the lower part of the colon (about 2 feet), and a colonoscopy provides a comprehensive view of the entire colon. In these tests, a small tube with a fibre-optic camera is inserted into the rectum, allowing for a detailed examination of the area, including the haemorrhoids.
What Are The Treatment Options For Haemorrhoids?
Hemorrhoids can be treated both at home and in a medical setting.
Pain Relief:
Soaking in a warm bath for at least 10 minutes daily can alleviate pain. Sitting on a warm water bottle may help with external haemorrhoid pain.
Over-the-counter (OTC) medicated suppositories, ointments, or creams can relieve burning and itching.
Fibre Supplements:
OTC fibre supplements like psyllium and methylcellulose can help soften stools if constipation is an issue.
Home Remedies:
Topical treatments such as hydrocortisone or haemorrhoid creams can reduce discomfort. Witch hazel pads are also effective.
Soaking the affected area in a sitz bath for 10-15 minutes daily can be beneficial.
Maintain good hygiene by cleaning the area with warm water and avoiding soap and harsh toilet paper.
Cold compresses can reduce swelling, and pain relievers like acetaminophen, ibuprofen, or aspirin can provide comfort.
Medical Procedures:
If home treatments are ineffective, a doctor may recommend rubber band ligation. This involves placing a rubber band around the haemorrhoid to cut off its circulation, causing it to shrink. This should only be performed by a healthcare professional.
Another option is injection therapy, or sclerotherapy, where a chemical is injected into the haemorrhoid, reducing its size.
Haemorrhoid Prevention
It's important to avoid straining during bowel movements to prevent or reduce the risk of haemorrhoids. Increasing your water intake can help keep your stool soft and stop it from hardening.
Using the bathroom as soon as you feel the urge to have a bowel movement can help prevent the development of haemorrhoids. Regular exercise can help avoid constipation, and limiting prolonged sitting is advisable, especially on hard surfaces.
Eating foods high in dietary fibre minimises the risk of haemorrhoids. Some good sources of dietary fibre are:
- Whole wheat
- Brown rice
- Oatmeal
- Pears
- Carrots
- Buckwheat
- Bran
Dietary fibre increases bulk in the intestines, which softens the stool and makes it easier to pass, reducing strain during bowel movements.
Complications
While complications from haemorrhoids are uncommon, they can occur and include the following:
- Formation of blood clots in the swollen vein.
- Bleeding from the affected area.
- Iron deficiency anaemia, which can result from blood loss.
- Infection in external haemorrhoid.
Development of skin tags, or extra skin, after an external hemorrhoid resolves.
Outlook
With appropriate treatment and adherence to your doctor's advice, there's a good chance of improvement. Regular exercise and avoiding prolonged sitting can further enhance your recovery and overall health.
Summary
Hemorrhoids, which are swollen veins in the anus and rectum, are common and often result from straining the rectal veins. Contributing factors can be chronic constipation, straining during bowel movements, a family history of haemorrhoids, or pregnancy.
In many cases, haemorrhoids resolve without intervention. Treatment typically alleviates symptoms, including warm baths and applying hydrocortisone or haemorrhoid creams or suppositories. Lifestyle changes like regular exercise, adequate water intake, and a fibre-rich diet can help ease constipation and reduce the likelihood of future haemorrhoid development.
Mobi Doctor offers practical solutions for managing health concerns like haemorrhoids, providing easy access to medical advice and support, helping you manage symptoms and preventing future occurrences from the comfort of your home.